Myanmar/Burma: Ensuring access to health care for conflict victims in Rakhine State
- 07/07/2016
- 0
By Mallika Panorat, ECHO, Thomas Reuters Foundation
Government-imposed restrictions on displaced Rohingya populations bar them from accessing health care
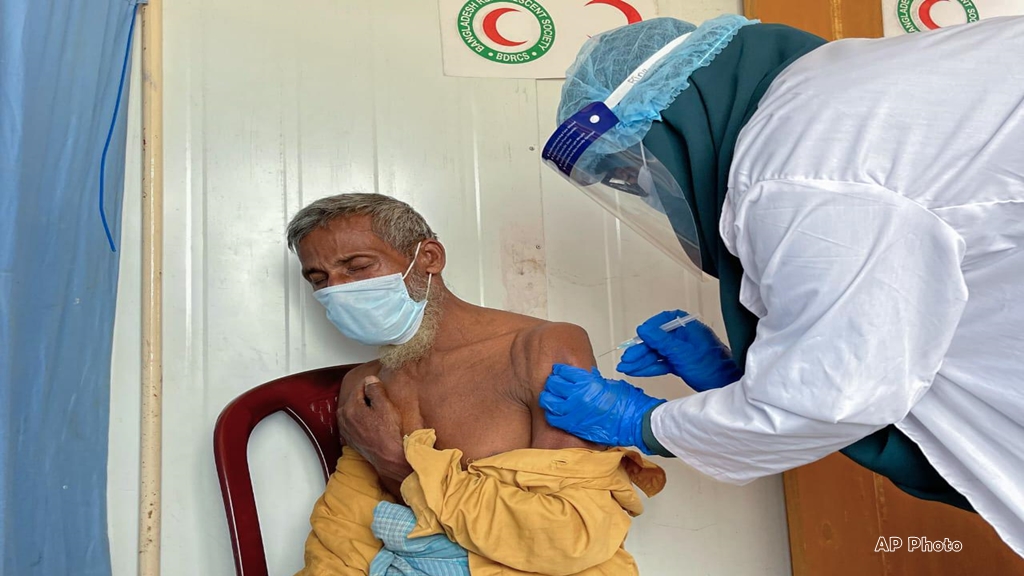
Four years after one of the worst outbreaks of intercommunal violence engulfed Myanmar’s Rakhine state in June 2012, more than 140 000 mainly ethnic Rohingya individuals remain displaced and live in camps. Government-imposed movement restrictions on Rohingya populations continue to bar them from accessing basic services, including health care. The European Commission is providing funds to ensure that access to medical services remains in place for the victims of conflicts and for the most vulnerable communities in the affected townships.
I grew up believing that everyone was entitled to basic health care services. It was only when I arrived in the Rakhine state’s township of Myebon that I realised how wrong I had been.
A serene township where villagers live on fishing and rice cultivation, Myebon is only accessible by a two-hour boat trip along a network of meadow-fringed rivers from the state capital of Sittwe. The natural beauty of the riverside settlement is however overshadowed by the presence of one of the country’s largest settlements for Internally Displaced Persons (IDPs)–the Taung Paw camp.
Created after the violent ethnic conflict in 2012, Taung Paw is home to more than 2 900 Rohingya people who sought shelter here after the clash between the Muslim minority and the Buddhist community. They are currently not allowed to leave the now dilapidated site without formal authorisation – a document that is not easy to come by since members of the religious minority are not recognised by the government as Burmese nationals.
“We are prohibited from venturing outside,” reveals Daw Phya Ma, a 32-year-old mother of four who has been living in the camp since 2012. “There is a military checkpoint just in front of the camp to make sure this rule is respected.” This restriction is in place without exception, not even for cases of medical emergencies. In practice, this means that residents are deprived of access to health care and other basic government services.
“As far as I can recall, at least 20 pregnant women have died in labour since we arrived here due to complicated referral procedures to other hospitals and other hardships,” adds Daw. This situation raises obvious humanitarian concerns about access to health care for the displaced people living in Rakhine, a state where deep-rooted ethnic polarisation prevails.
Thanks to funding from the European Commission, Relief International introduced a health care project in several camps and remote villages across the coastal state to ensure that the victims of conflicts and the most vulnerable populations have access to basic health services. Within this programme, an in-camp clinic was opened in Taung Paw. Dr Aye Moht Moht is a 25-year-old physician from Yangon and the camp’s only female doctor. She was invited to join the Relief International team as a practicing physician in the framework of a gender-sensitive approach to offer medical care to female patients with a specific focus on antenatal care for pregnant women. “Since I started working here, we have seen more and more female patients, especially pregnant women, coming to the clinic,” explains Dr Moht in the bustling single-room clinic. “They are happy to see a female doctor because they feel more comfortable being physically examined or sharing their concerns with me.”
Besides providing medical consultations, the team also refers patients to a more equipped health facility when needed. This process can make the difference between life and death in times of emergency, as Rohingya patients cannot access these facilities on their own. “On a December day last year, a 36-week pregnant woman came to the clinic saying she had persistent headaches and felt dizzy,” recalls Dr Moht. “After some tests, we realised that we needed to immediately request permission for an emergency referral to Sittwe Hospital.”
Dr Moht and her team continued to monitor the patient’s blood pressure throughout the night, until at sunrise a boat finally arrived to collect the woman. Upon reaching the hospital in Sittwe, the patient was diagnosed with pre-eclampsia and low levels of amniotic fluid. The availability of more advanced medical equipment proved critical to save the lives of both mother and baby.
Back in the waiting room at the clinic, Daw Phya Ma is all praise for the medical staff looking after her. “It’s great that we can now come here and receive treatment,” she says. “Because of the restrictions on our freedom of movement outside the camp, we are completely dependent on this clinic.”
I leave Taung Paw camp with a flare of hope, knowing the necessary medical support for victims of conflicts is ensured despite all the obstacles that still exist. As we bid farewell Dr Moht tells me:
“They are all my patients.”
The story was written by Mallika Panorat, Information and Communication Assistant for Asia-Pacific, European Commission’s humanitarian aid department.